Healthcare license verification is the essential process of confirming a medical professional's legal authority to practice by checking their credentials directly with the primary issuing source. Workers in healthcare who operate without a proper, active license pose immense risks to healthcare organizations, with consequences including
- regulatory fines from audit findings;
- increased liability from licensure lapses; and
- severe patient safety risks due to unmonitored adverse actions.
Medical staff services and compliance teams should consider implementing robust, repeatable checking procedures to mitigate these operational threats. If you are a healthcare employer, here’s what you need to know.
License Verification Requirements, Who Sets Them
The foundation of any medical credentialing program begins with understanding the core regulatory bodies: State licensing boards are the ultimate authority, granting permission to practice within their jurisdiction. Every state board sets unique requirements for issuing, renewing, and maintaining credentials, and every hospital and staffing firm needs to check these individual state databases to confirm a practitioner's active status.
Beyond state boards, the Centers for Medicare & Medicaid Services (CMS) establishes a strict baseline for licensed personnel. Under the eCFR 42 CFR 482.11 licensing baseline, hospitals must verify that all personnel hold the necessary licensure and meet applicable state or local standards. If healthcare employers hire uncredentialed staff, per the CMS, they could place their federal funding at risk.
Additionally, a major evaluating organization called The Joint Commission requires hospital HR teams to verify a worker's qualifications directly with the original licensing board when they are first hired and again when their license is up for renewal. When inspectors visit the hospital, they want to see clear, written proof that the staff actually checked the license by either making a documented phone call (evidenced by a written audit trail or log of the call) or using a secure website.
Primary Source Verification, What Counts, What Evidence Proves Completion
“Primary source verification” (PSV) means cross-checking an employee’s credentials with the original source or an approved agent. Employers must use methods approved by the Joint Commission to verify credentials; these methods include direct correspondence, documented phone verification, secure electronic verification, or reports from a qualified Credentials Verification Organization (CVO). Simply gathering credentials is not enough; the method of confirmation matters heavily.
Auditors who conduct a Joint Commission review also look closely at the documentation retained in the credential file. Documentation should clearly show the date of the verification, the name and role of the person completing the verification, the specific items verified, and the ultimate verification results.
A common pitfall in the credentialing process is relying on physical documents provided by the applicant: A license copy alone does not meet the intent of primary source verification. Because physical copies can be easily forged or outdated, accrediting bodies demand direct confirmation from the issuing entity.
| PRIMARY SOURCE VERIFICATION | ||
|---|---|---|
| Verify the credential with the original issuing source, or an approved equivalent source | Acceptable methods: Direct correspondence, Documented phone verification, Secure electronic verification, Qualified CVO report | Retain: date, source, result, reviewer, and proof of completion. A license copy alone is not enough. |
Primary Source Verification vs. Credential Verification
People often use the terms "credential verification" and "primary source verification" to mean the same thing, but they are very different.
“Credential verification” is a broad term for checking a person's background, education, or work history. In many regular businesses, this might just involve looking at a physical copy of a college degree or calling a past employer to confirm dates of work.
Primary Source Verification is a much stricter process designed specifically for healthcare: Instead of accepting a physical copy of a license from the worker, PSV means the facility goes directly to the official group that created the license in the first place.
The difference between the two is crucial: If a hospital just does basic credential verification by looking at a paper license, they might miss the fact that the worker was suspended just last week. PSV ensures the facility gets the most accurate, up-to-date information.
The Costs of Non-Compliance
If a healthcare employer fails to maintain a rigorous license verification program, they may face severe financial and legal consequences.
- If a facility employs an individual who is on the federal excluded list, the Office of Inspector General (OIG) can impose fines of more than $25,000 for each item or service provided by the excluded worker.
- If an unverified employee harms a patient, the facility can face negligent credentialing lawsuits. Courts often hold facilities responsible if they discover the hospital failed to perform basic primary source verification.
- Organizations like The Joint Commission can revoke a hospital's accreditation if surveyors find consistent gaps in credentialing records, which can lead to a loss of Medicare and Medicaid funding and force a facility to close its doors entirely.
Step-By-Step Workflow, From Application Through First Shift
A resilient hiring process with robust primary source verification requires multiple touchpoints, beginning with a pre-offer check. Before extending an employment offer, organizations should consider verifying the primary source credential to ensure the candidate is legally eligible for the role.
A pre-start recheck is the next critical phase in the workflow. Timing checks before the offer and immediately before the first shift ensures that no disciplinary actions have occurred during the transition period. By day one, the organization should enforce a strict credential file completeness standard, with full documentation of all verification steps before the practitioner assumes their duties.
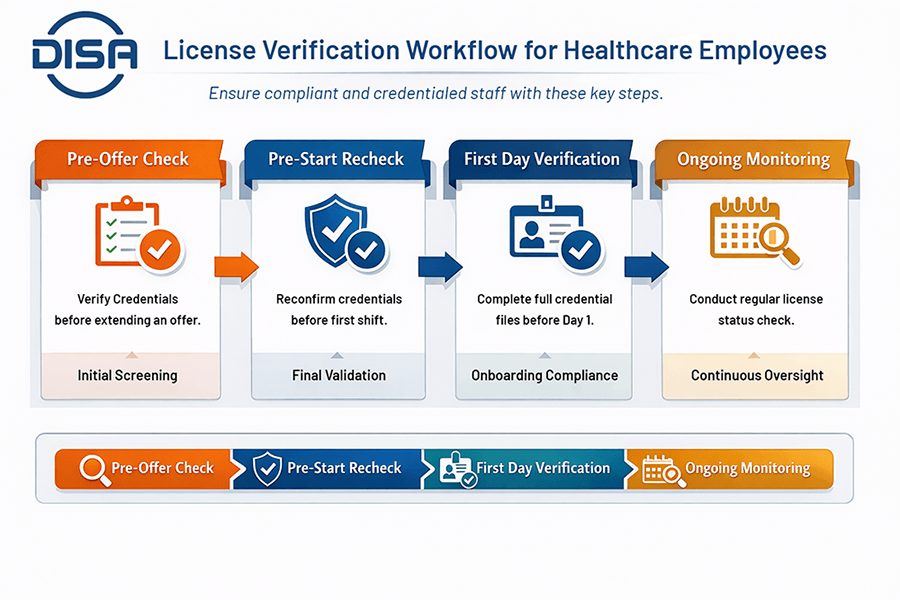
Ongoing Checks, Set Frequency by Role Risk
Verification is not a one-time event; healthcare employers should also track their employees’ license renewals and conduct periodic, monthly rechecks to ensure their staff remain compliant throughout their tenure. Different clinical roles carry different risk profiles, so the frequency of checks should align closely with the risk level of the position.
| Worker type | Primary license source | Required related checks | Timing and frequency | Evidence to retain |
|---|---|---|---|---|
| Nurses, LPN, APRN | Nursys or state board | OIG LEIE | Pre-offer, pre-start, then scheduled rechecks | Primary source verification (PSV) record, screenshot or confirmation number, dates |
| Physicians, PAs | State medical board, Federation of State Medical Boards (FSMB) data sources as applicable | National Practitioner Data Bank (NPDB) query for privileging, Office of Inspector General List of Excluded Individuals and Entities (OIG LEIE) | Initial privileging, every 2 years for hospitals | NPDB query proof, PSV record plus dates and reviewer |
| Allied health, techs | State board or cert body | OIG LEIE | Pre-offer, pre-start, then scheduled rechecks | PSV record, expiration plan plus escalation notes |
To manage this process efficiently, teams should consider using monitoring triggers and automated status-change alerts to notify HR the moment a state board updates a license status or posts a disciplinary action.
Frequently Asked Questions
What counts as primary source verification for healthcare licensure?
Primary source verification requires verifying a reported qualification directly with the original issuing source or an approved agent. Acceptable methods include direct correspondence, documented phone verification, secure electronic verification, or reports from a qualified CVO meeting Joint Commission requirements.
A proper audit trail should show the date of verification, the person completing the verification, the specific items verified, and the verification results. A license copy alone is not considered acceptable proof.
Hospitals must query practitioners at their initial application for privileges, and then every two years while they remain on staff. Queries are also required when a practitioner is expanding or adding new privileges.
Routine checks of the OIG LEIE help avoid severe civil monetary penalties (such as $25,595 per violation for employing or contracting with an excluded individual, or $127,973 for knowingly making false statements to participate as a provider) associated with employing excluded individuals or entities. Employing excluded individuals puts federal healthcare program funding at immediate risk.
Nursys serves as a national database that covers the verification of nurse licensure, discipline records, and practice privileges across participating jurisdictions, including all NLC states.
Note that employers cannot rely universally on the Nursys database for APRN verifications because not all state boards submit advanced practice license information to the Nursys system.
The Nurse Licensure Compact (NLC) allows nurses to practice in other participating NLC states without obtaining additional, separate licenses, which streamlines the verification process through a centralized database.
The Interstate Medical Licensure Compact (IMLC) provides an expedited pathway to licensure for qualified physicians who want to practice in multiple states, by simplifying the process of acquiring individual, separate licenses in participating states.
Any adverse actions, sanctions, suspensions, revocations, or expired statuses require immediate escalation to compliance or risk teams prior to allowing a practitioner to work.
A thorough report should include the license number, license type, issue date, expiration date, and any records of disciplinary actions, sanctions, suspensions, or revocations.
How DISA Can Help
At DISA Global Solutions, we understand the complexities of managing compliance and safety in the healthcare industry. DISA supports professional license verification workflows by verifying credentials directly with accrediting bodies or professional associations. Our reports return crucial data points, including the license number, license type, issue date, expiration date, and any disciplinary actions, sanctions, suspensions, or revocations.
DISA’s comprehensive services are designed to support healthcare organizations in their journey toward full regulatory compliance and operational efficiency. With our comprehensive support, you can confidently navigate the complexities of healthcare compliance and protect your organization from liability. Contact us today to request a demo for DISA professional licenses and healthcare compliance programs, and learn how we can help your facility achieve true operational excellence.
DISA Global Solutions aims to provide accurate and informative content for educational purposes only and does not constitute legal advice. The reader retains full responsibility for the use of the information contained herein. Always consult with a professional or legal expert.






